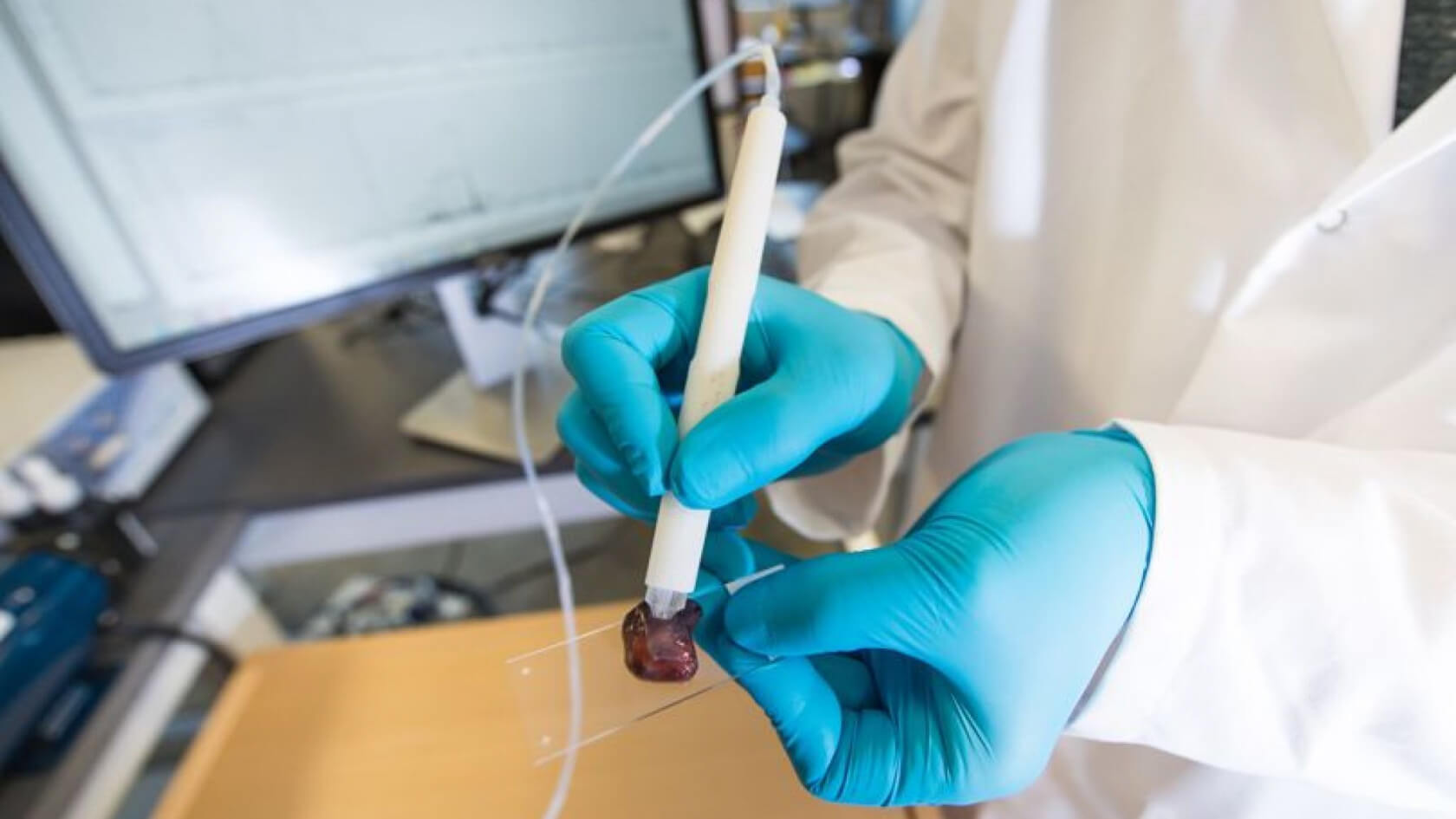
For all the technical advances made in the world of medicine, identifying and removing cancerous tumors from patients remains a slow and unreliable process. But scientists at the University of Texas have created a pen-sized device that can detect cancerous tissue in just ten seconds.
Removing all traces of cancer is an extremely delicate operation; leaving any small pieces behind means a second procedure, but surgeons don't want to remove too much healthy tissue and risk damaging organs. A process called frozen section analysis can be used to identify cancerous cells, though it takes time and is not always accurate.
But researchers say the MasSpec Pen can help surgeons remove "every last trace of the disease." Once the device touches a suspected area of cancer, a tiny droplet of water leaves the pen tip and sits on the tissue for three seconds. The water is then sucked up by the pen and travels down a tube into a mass spectrometer, where the molecules are analyzed to give a "fingerprint" of the tissue. This shows if traces of cancer are present.
"This is a very gentle chemical process, and what is incredible and exciting is that it causes no obvious harm to the tissue. You can think about it in the same way that water extracts caffeine from coffee powder, we use water to extract molecules from tissue," said the study's author, Dr. Livia Schiavinato Eberlin, an assistant professor of chemistry at the University of Texas.
In the study (published in Science Translation Medicine) researchers tested 253 human tissue samples from cancer tumors and compared them to samples of healthy tissues. They found the pen's overall accuracy to be 96.2 percent.
Right now, it can analyze tissue patches measuring 1.5mm (0.06) inches across, but a more refined version has been developed that can examine finer areas of just 0.6mm.
While the small pen itself doesn't cost much to manufacture, the large, expensive mass spectrometer is the main stumbling block. "We're visioning a mass spectrometer that's a little smaller, cheaper and tailored for this application that can be wheeled in and out of rooms," said Dr. Eberlin.
Clinical testing on humans is set to begin next year.